AI & Health Outcomes: Mapping the Rural Digital Divide
Investigating how geographic barriers prevent rural communities from health gains afforded by access to AI healthcare superstructures.
Overview
The Problem
AI benefits are concentrated in urban regions of the us, leaving rural populations in "tech-care deserts."
The Impact
Demonstrated that distance to care can be as much of a digital barrier as a physical one, quantifying how geographic isolation limits access to advanced health care.
- My Role: Lead Researcher (Directed Research Group, UW).
- The Toolkit: Quantitative Analysis in R (sf, ggplot2), Overleaf/LaTeX, CDC & USDA Public Datasets.
Understand
Designing for health equity requires looking at the infrastructure of access. If a patient lives 50 miles from a healthcare network that leverages AI tools and lacks high-speed broadband, the "user journey" for a life-saving diagnosis is fundamentally broken before it begins.
The Strategic "Why"
I performed a Literature Review of 25 peer-reviewed research articles to identify existing friction points, relationships between health and space, and how spatial outcomes often drive social disparity. This research revealed that AI models are often trained on urban data, leading to a geographic disconnect that alienates rural users.
Research
Methodology & Data Rigor
- Data Engineering: Loaded and cleaned multi-source public datasets (USDA, CDC, NHANES) using R.
- Controlling for Confounds: Isolated variables like Socioeconomic Status (SES) to ensure findings weren't just a proxy for wealth.
- Spatial Regression: Used `sf` and `sfdep` packages to visualize the correlation between mileage and health risk.
Research Artifacts
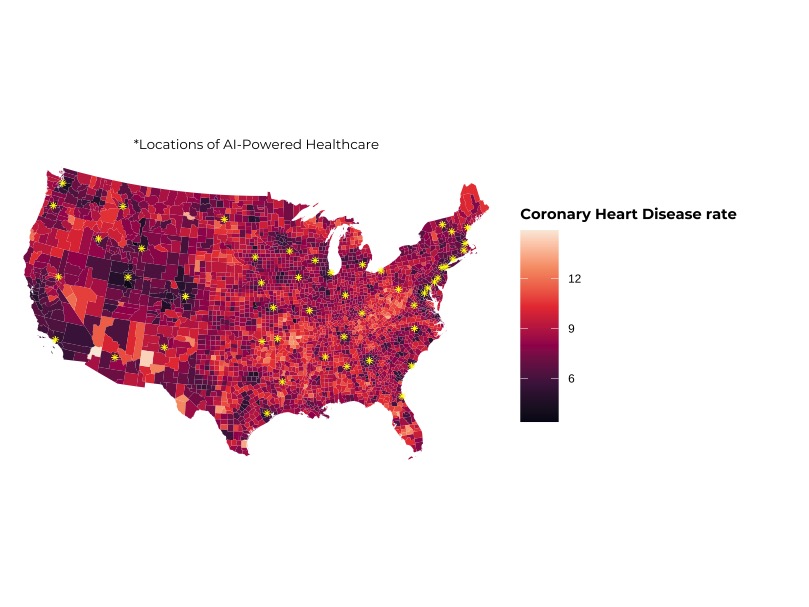
The yellow stars on this cloropleth plot are the locations of what I have referred to as "AI Superstructures" and the surrouding plot shows the incidence of coronary heart disease.
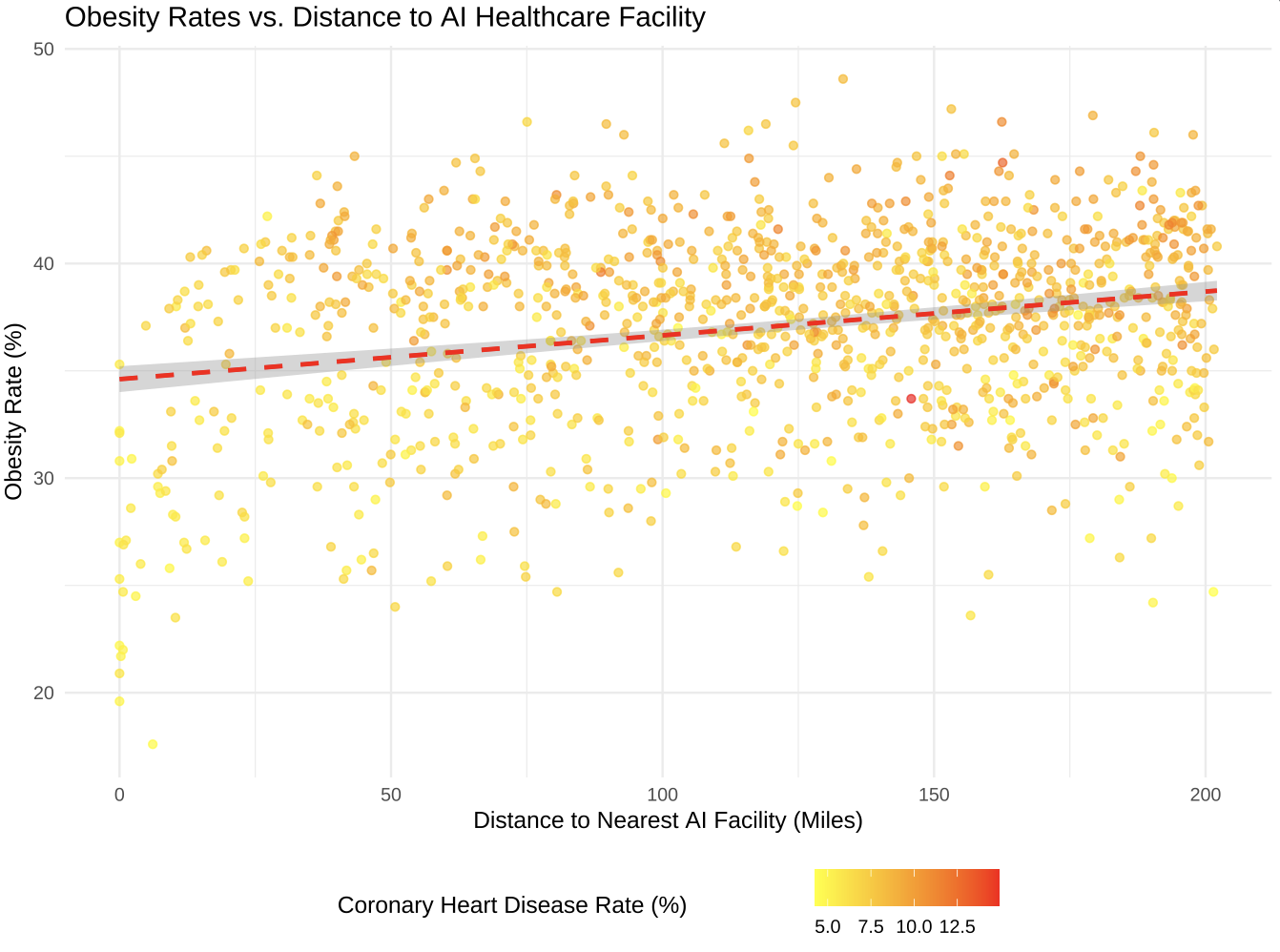
The scatter plot illustrates a positive correlation between the distance to the nearest AI facility and obesity rates, suggesting that as distance increases, the percentage of obesity also tends to rise.
Outcome & Impact
Infrastructure is the primary gatekeeper of health equity. When AI tools are tethered to urban digital standards, they inadvertently exclude rural communities, deepening the existing divide in health outcomes.
1. The Distance Gap
Statistical analysis showed a correlation between distance from healthcare "superstructures" and higher health risks. This identifies a geographic penalty where physical isolation limits access to advanced diagnostic networks.
2. The Trust Barrier
Literature synthesis suggests a socio-technical divide: rural populations may exhibit hesitation toward "urban-centric" tech. This highlights that social and cultural familiarity can be as significant a hurdle as technical infrastructure.
3. Connectivity Bottleneck
Broadband scarcity acts as a gatekeeper for advanced care. Data trends suggest that limited connectivity prevents the deployment of high-bandwidth AI tools, impacting the health outcomes of rural communities by stalling access to higher tech health care for early detection/diagnosis and treatment.
Takeaways
The Big Picture
This project shifted my perspective on research: it’s not just about interface design—it’s about the infrastructure of access. For AI to be equitable, the environmental and technical constraints of rural communities must be treated as primary requirements from Day 1.